Understanding Diabetes and Skin Health
Diabetes affects every part of your body, including your skin. In fact, skin problems are often the first visible signs of diabetes. High blood sugar levels can cause damage to blood vessels and nerves, reducing circulation and impairing the skin's ability to heal. This makes people with diabetes more susceptible to various skin conditions, from minor irritations to serious infections. Understanding the connection between diabetes and skin health is crucial for prevention and early intervention.
Approximately one-third of people with diabetes will experience a skin disorder at some point in their lives. Some skin conditions are caused by diabetes itself, while others are related to complications of the disease. The good news is that most diabetes-related skin problems can be prevented or treated successfully when caught early. By maintaining good blood sugar control and following a proper skincare routine, you can significantly reduce your risk of developing serious skin complications.
Regular blood sugar monitoring is essential for overall health
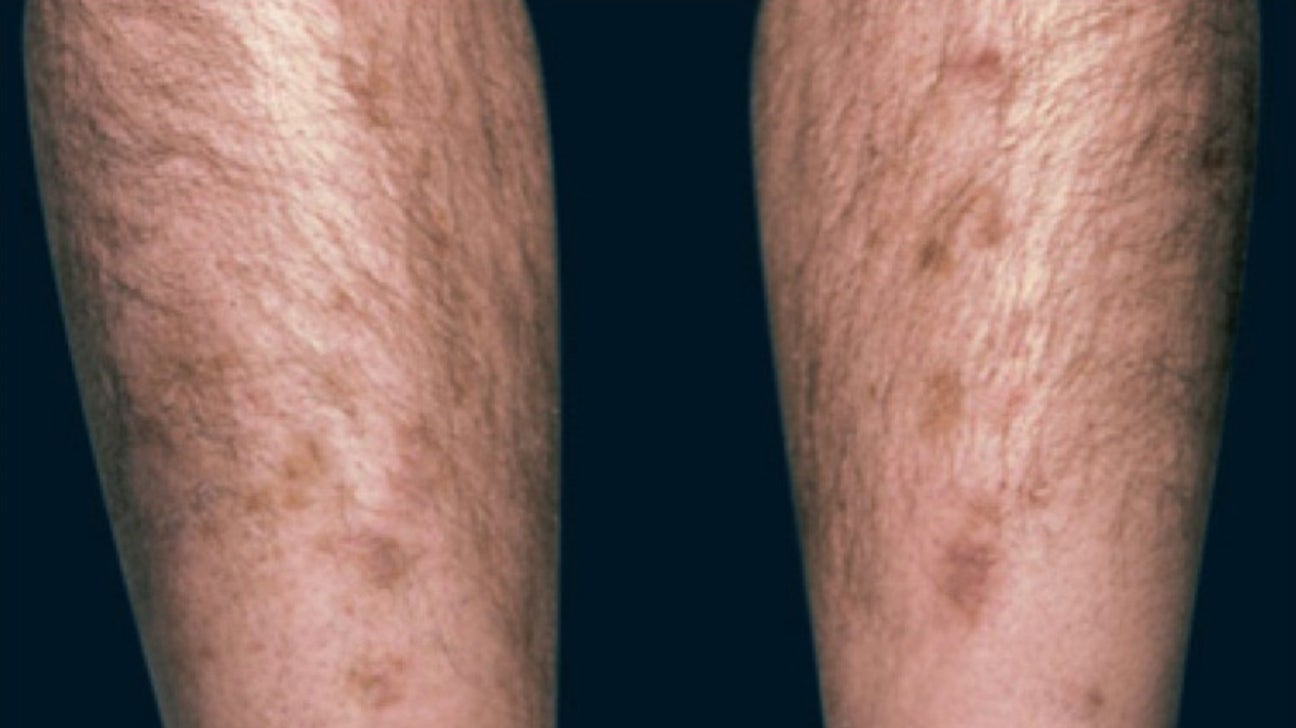
Diabetic dermopathy is a common skin condition in diabetics
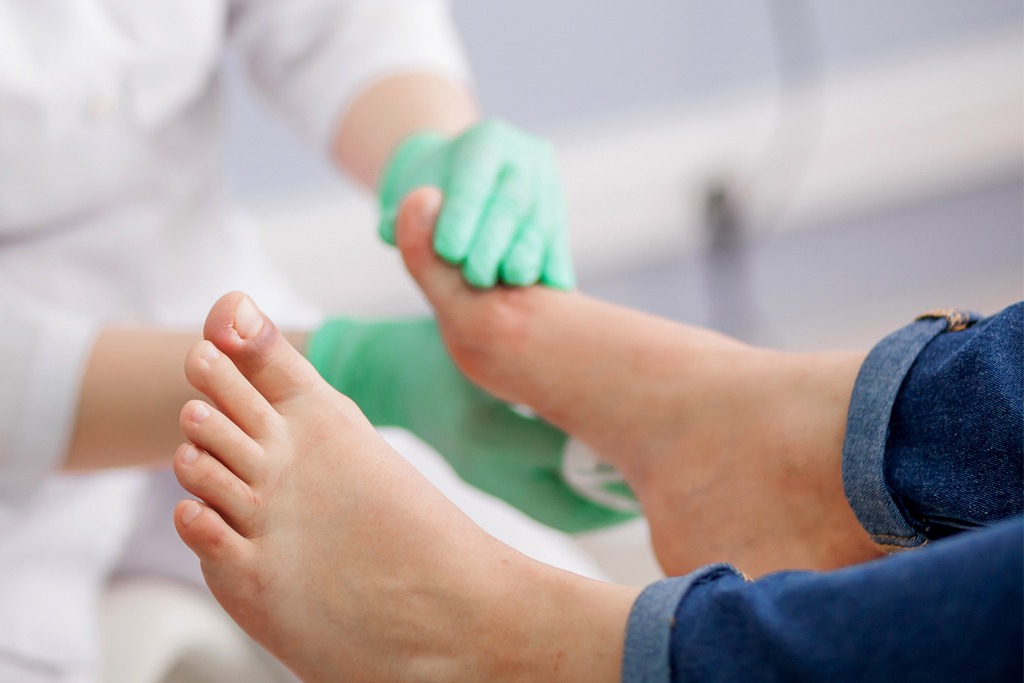
Regular foot exams are crucial for diabetic patients
Common Skin Conditions in Diabetics
People with diabetes are prone to several specific skin conditions. Diabetic dermopathy, often called "shin spots," appears as light brown, scaly patches on the shins and is caused by changes in small blood vessels. While harmless, these spots can be a warning sign of diabetes. Necrobiosis lipodermatitis is a more serious condition that causes reddish-brown patches that can ulcerate. Both conditions are related to changes in the blood vessels and collagen in the skin.
Other common skin issues include fungal infections such as athlete's foot, which thrives in the warm, moist areas between toes. Bacterial infections like boils, folliculitis, and carbuncles are also more common in people with diabetes due to reduced immune function. People with diabetes may also experience dry skin, particularly on the legs and feet, which can lead to cracking and increase the risk of infection. Being aware of these conditions allows for early detection and prompt treatment.
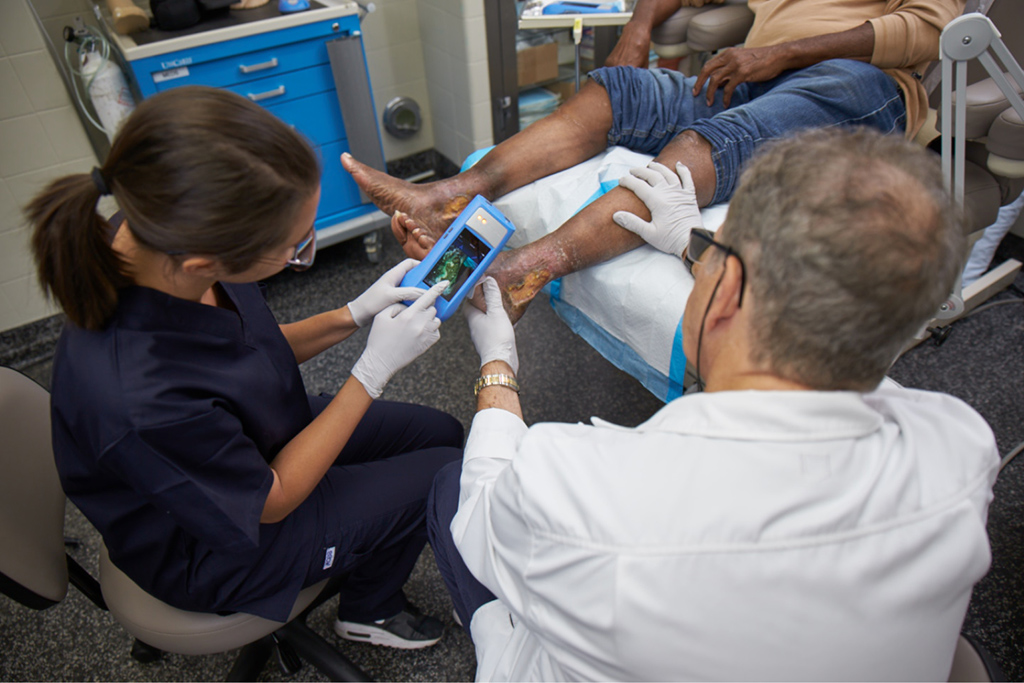
Proper wound care is essential for diabetic patients

Nutrition plays a key role in managing diabetes and skin health
The Importance of Foot Care
Foot care is perhaps the most critical aspect of skin health for people with diabetes. Due to nerve damage (neuropathy) and poor circulation, injuries to the feet may go unnoticed and heal slowly. A small cut or blister can develop into a serious infection if not treated promptly. This is why daily foot inspections are absolutely essential for anyone with diabetes. Check your feet every day for cuts, blisters, redness, swelling, or any signs of infection.
Proper foot care includes keeping your feet clean and dry, moisturizing but avoiding the areas between toes, wearing comfortable, well-fitting shoes, and never walking barefoot. It is also important to have your feet examined by a healthcare professional at least once a year, or more frequently if you have a history of foot problems. Any foot sore or wound that does not begin to heal within a few days should be evaluated by a doctor immediately. With proper care, most diabetes-related foot problems can be prevented.
Warning: Seek Immediate Medical Attention
If you notice any signs of infection on your feet, such as increased redness, warmth, swelling, pus, or fever, contact your healthcare provider immediately. Do not attempt to treat foot infections at home. Early intervention is crucial to prevent serious complications, including amputation.
Managing Blood Sugar for Healthy Skin
Maintaining stable blood sugar levels is fundamental to preventing diabetes-related skin problems. When blood sugar levels are consistently high, it can lead to dehydration, which causes dry skin and poor wound healing. High glucose levels also provide food for bacteria, increasing the risk of infections. By keeping your blood sugar within your target range, you can significantly reduce your risk of skin complications.
Following your diabetes management plan is essential. This includes taking medications as prescribed, monitoring your blood sugar regularly, eating a balanced diet, and exercising regularly. When your blood sugar is well-controlled, your circulation improves, your immune system functions better, and your skin can heal more effectively. Work with your healthcare team to develop a diabetes management plan that works for you and helps maintain both your overall health and your skin health.
Daily Skincare Routine for Diabetics
Establishing a proper daily skincare routine is essential for people with diabetes. Start by keeping your skin clean and moisturized, as dry skin is more prone to cracking and infection. Use mild, fragrance-free soaps and cleansers that won't irritate your skin. After bathing, gently pat your skin dry and apply a moisturizer while your skin is still damp to lock in hydration. Focus on areas prone to dryness, such as legs, feet, and elbows.
Protect your skin from injury by wearing comfortable, protective clothing and shoes. Avoid tight clothing that can restrict circulation. Use sunscreen with at least SPF 30 to protect against sun damage, which can cause skin cancer and worsen existing skin conditions. Stay hydrated by drinking plenty of water throughout the day. If you notice any skin changes, such as new spots, rashes, or wounds that won't heal, consult your healthcare provider promptly.
Daily Inspections
Check your feet and skin daily for any cuts, blisters, redness, or changes. Early detection of problems leads to better outcomes.
Blood Sugar Control
Maintain stable blood glucose levels through diet, exercise, and medication as prescribed to reduce skin complications.
Moisturize Regularly
Keep your skin moisturized to prevent dryness and cracking, especially on feet and legs.
When to See a Doctor
While minor skin irritations can often be managed at home, certain symptoms require prompt medical attention. You should see a doctor if you notice any skin infection, including increased redness, warmth, swelling, pain, or pus. Any wound that does not start to heal within a few days needs professional evaluation. Persistent dry skin, itchy rashes, or new skin growths should also be discussed with your healthcare provider.
Regular check-ups with a dermatologist can be beneficial for people with diabetes, especially those with a history of skin problems. Your doctor can help you develop a personalized skincare plan and address any concerns before they become serious. Remember, prevention and early intervention are key to maintaining healthy skin while managing diabetes.